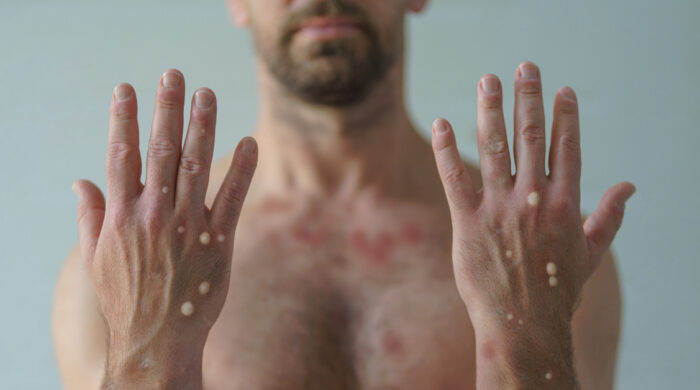
Until this summer, most Americans had never heard of Mpox (formerly known as monkeypox). By late August 2022, nearly 20,000 cases had been diagnosed in the U.S., with close to 50,000 worldwide. Mpox seems poised to launch a new pandemic. Just how worried should you be?
What is Mpox?
Mpox was first identified in 1958 in colonies of monkeys kept for research, but the source of disease remains unknown. Mpox is caused by a virus that belongs to the same group (Orthopoxvirus) as smallpox. Unlike smallpox, Mpox is rarely fatal. The severity of the disease is often closer to that of chickenpox, although it is unrelated to chickenpox. “Pox” describes any disease that produces pimple-like rashes.
Mpox was first recorded in a human in 1970, but until very recently, it was reported in central and west African countries. Beginning in May of this year, Mpox outbreaks began in the U.S. and other countries. On August 4, 2022, the U.S. federal government declared Mpox a public health emergency.
What’s the risk?
Unlike COVID, which is transmitted through respiratory droplets, Mpox spreads through close, personal contact with the scabs or fluid contained in the lesions that form on the skin of an infected person. Most commonly, this occurs during skin-to-skin contact, but can result from shared clothes and bedding.
So far, men who have sex with men have been most affected by the Mpox epidemic. People who are sexually active, gay, or bisexual, may also be at high risk.
However, Mpox is not restricted to any particular group. Any person who has been in any kind of physical contact with an infected person is also at risk for infection.
Symptoms of Mpox
A person who is infected with Mpox can take between 3 – 17 days to develop symptoms. Most infected people will develop a rash, followed by flu-like symptoms. Symptoms can include:
- Rash
- Fever
- Headache
- Muscle aches
- Swollen lymph nodes
- Fatigue
- Respiratory symptoms
Patients are contagious from the first appearance of a rash until the last scab heals. The illness usually lasts two to four weeks. Although the rash can be very painful, most Mpox cases can be managed at home. Anyone who is immune-compromised, pregnant, or elderly, and children under the age of eight may be at higher risk for severe illness.
Mpox vaccination
So far, no vaccine has been developed specifically for Mpox. However, because the two diseases are related, smallpox vaccines may prove effective in preventing Mpox infections. These vaccines are currently being tested in humans for safety and their effectiveness against Mpox. But it is suspected that they may have contributed to widespread immunity that prevented Mpox from spreading in the past. Smallpox vaccinations stopped being mandatory decades ago (the disease was eliminated in 1977), possibly leaving unvaccinated younger generations more susceptible to Mpox infection.
There are two types of smallpox vaccine. ACAM2000 is introduced through a scratch in the skin. It forms a “pock” at the inoculation site and can leave a scar. As of this writing, it is not yet publicly available in the United States.
JYNNEOS is a vaccine administered by injection as a two-dose series, and as such is the primary vaccine being used in the United States during this outbreak. Supplies of JYNNEOS are extremely limited and for now it is only available to individuals who have been exposed to Mpox or are at high risk for exposure, such as healthcare workers who treat Mpox. If you think you might be eligible, you can contact your primary care provider for help obtaining a vaccination.
Preventing and treating Mpox
The best method of prevention is to avoid close contact with anyone who has a rash. If you travel, avoid contact with rodents and primates.
If you think you’ve been exposed to Mpox or develop an unfamiliar rash, do not ignore it. Contact your primary care provider. Let them know up front that you are concerned about Mpox, because many doctor’s offices and clinics have established protocols for dealing with Mpox. Avoid close contact with others until you can be tested or diagnosed.
If you are infected with Mpox, follow your primary care provider’s instructions. Isolate at home and avoid close contact with others, including pets, until your skin is completely healed from the rash. In most cases, the illness can be managed at home with over-the-counter medicines for pain. For vulnerable populations and in more severe cases, the antiviral medication tecovirimat (TPOXX) may be helpful.
Although few doctors in the U.S. have ever seen a patient with Mpox, recognition of the disease, access to testing and vaccines are improving, as is the quality of available information. As with any outbreak, the circumstances around Mpox are rapidly evolving. The CDC maintains a web page with information on Mpox, but you can contact your primary care provider for help with your specific questions.
For more information and updates on the current status of Mpox in the U.S., visit the CDC website.