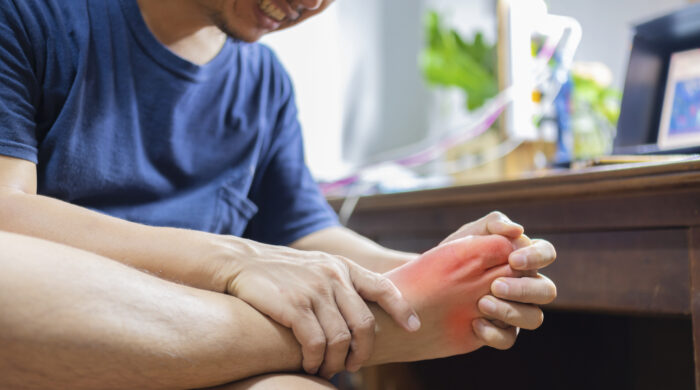
Gout is the most common form of inflammatory arthritis. Not only can it be extremely painful, but left undiagnosed, it can lead to more serious health problems down the line.
Some 8 million Americans suffer from gout, which typically develops in men during their thirties, and in women after menopause. However, it can occur in anyone, and signs of gout may appear as early as the teen years.
Early intervention is key to diagnosing and effectively treating gout at any age. Here’s what you need to know.
Symptoms of Gout
For some patients, the underlying conditions of gout may be present without causing any symptoms at all. But for most patients with the condition, gout shows up in intermittent flare-ups. In the long-term, persistent gouty arthritis can lead to chronic pain and disability.
The symptoms of gout appear most often as severe, painful inflammation of the big toe joint. But while it is most common in the joints of the extremities (such as hands and feet), gout can occur anywhere in the body.
“It’s like peeling your skin off and pouring acid on it. Women say it’s worse than childbirth,” said Dr. Jeff Peterson, Rheumatologist at Western Washington Medical Group’s rheumatology clinic in Bothell. Flare-ups can last for days, during which time the pain can make it impossible to move or even touch the affected joint, which becomes hot, red, and swollen. In some cases, the inflammation is severe enough to cause peeling skin.
Causes of Gout
“Gout is a systemic, chronic disease that affects the joints and organs” by depositing sodium urate crystals, said Peterson. When the body produces sodium urate at a higher level than normal, or the kidneys fail to process it quickly enough, crystals build up, deposit in the joints and organs, and cause damage.
Gout flare-ups occur when the immune system responds to the crystal deposits. Sometimes crystals get coated in protein and become invisible to the immune system. When this happens, joints can become severely damaged without the patient experiencing any flare-ups.
Although flare-ups are painful, they are usually what leads to a diagnosis. Asymptomatic cases that go undiagnosed can have serious long-term impacts.
“Even when they don’t cause pain, the crystals are still inflammatory. They can still nibble away at the bone and tendons. They can still invade tissues and cause them to not function properly,” said Peterson. Gout can inflame tissues in the eye, kidneys, prostate or liver, causing those organs to malfunction.
Further, this long-term inflammation leads to increased production of cortisol, also know as the ‘stress hormone.’ “Cortisol is like a steroid that helps to control inflammation. But it also leads to weight gain, high blood pressure, diabetes and high cholesterol,” Peterson said, and “can predispose people to metabolic syndrome,” which can increase a person’s risk of having heart disease or a stroke.
That being said, lifestyle changes and appropriate treatment can help manage the condition and prevent flare-ups.
Diagnosis and Treatment
Gout is usually diagnosed by a blood test that is not part of the standard panel. A new CT imaging test will actually show the crystal buildup on the affected joint to confirm the diagnosis.
There is no official guideline for screening for gout, so many primary care providers don’t routinely test for it. As result, it often goes undiagnosed until the patient has a painful flare-up. Gout is becoming more common, so any concerns should be brought up with your healthcare provider, who can refer you to a rheumatologist as needed.
“Gout is easily treated if you’re diligent. Treatment makes lives much better and can prevent other illnesses like metabolic syndrome,” said Peterson. The primary treatment for gout is medication.
Although it is not a substitute for medication, taking Vitamin C can have a minor beneficial effect. Gout patients should also avoid foods that are rich in purine, such as seafood and red meat. In severe cases where regular medication is not effective, infusion therapy drugs can be administered to reduce inflammation.
Prevention
“Unfortunately, there is not much you can do to prevent gout,” said Peterson. Genetic predisposition is the primary determinant for gout, although sometimes it can develop as a result of kidney disease. Temporary gout-like flare-ups can also occur during chemotherapy.
Lifestyle changes can help. Diet does not cause gout, but it can exacerbate it somewhat.
“Alcohol and high fructose corn syrup are the two big bugaboos for gout,” Peterson said. Extreme obesity can also contribute to development or worsening of the condition.
Since there is not much individuals can do to reduce their chances of developing gout, early detection is the focus. Individuals with a family history of gout should request screening from their primary care provider. If needed, they can receive a referral to a rheumatologist for further assessment.
Regardless of family history, no one should ignore sudden, painful joint inflammation. Even if it goes away in a couple of days, joint flare-ups should be reported to your primary care provider so appropriate treatment options can be discussed.
Gout is a chronic condition. Medication can dissolve existing crystals, but without ongoing treatment, new crystals will form. Fortunately, by adhering to a consistent treatment plan, and working with a supportive provider, gout can go into remission and future flare-ups may be prevented entirely.
Clinical Research Studies for Gout
WWMG offers a clinical research study for Gout. Learn more and enroll today:
https://www.wwmedgroup.com/gout-clinical-research-studies
If you have a family history of gout or are experiencing painful joint flare-ups, contact a WWMG primary care provider or rheumatologist today. We can help.